
The following article is contributed by Dr. Anna Cabeca, internationally recognized gynecologist and sexual health expert.
From Desert-like to Dessert-Like!
(The Vulvar & Vaginal Dryness Solution You’ve Been Looking For)
By Dr. Anna Cabeca
As an internationally recognized gynecologist and sexual health expert, I saw women in my practice on a daily basis who suffered unnecessarily from the pain and embarrassment of vaginal dryness. This pelvic health condition affects more women, of all ages, than most realize and sadly many feel they have no other option but to suffer in silence and accept the discomfort as their new “normal”.
Ladies, I am here to share with you what I often say to my patients – please be more gentle and loving with yourselves! There are now effective treatment options available, containing DHEA and some other key ingredients, which not only lessen the discomfort but also help to restore vaginal health and vitality.
Let’s take a look at the potential causes and symptoms of vaginal dryness and why it is key as women to address this often disregarded, under-attended to, and yet life-affecting issue…
What’s going on with my skin “down there”?
Even younger women can have dry and irritated tissue around the vulva as well as the vagina. Women who take the pill for example or those that take any number of other medications may experience a drying side effect in their most sensitive feminine zone. (1)
And older women, those going through peri-menopause or menopause, will likely experience vaginal dryness and other symptoms due to natural hormone decline.
We have a number of vital sexual hormones that yes, alas…start to decline as early as our thirties. Progesterone starts to decline, along with estrogen and also our androgens. Androgens include the sex hormones DHEA and testosterone (yes, women have – and need – testosterone!).
Receptors for these hormones are found all over in the vulva, clitoris, urethra, vagina, and uterus; as well as throughout the musculature of our pelvic floor. That is why as we age we begin to see a weakening of our pelvic floor (and that is important as our diminishing pelvic musculature health is why we start to leak when we laugh, cry and squat!).
Natural hormone decline causes symptoms which can greatly impact our lives…
Here’s what you may notice physically:
- Diminished natural lubrication
- Yes, things can start to hurt…whether that discomfort occurs during sexual intercourse or while simply doing things we enjoy, like riding a bike or doing our daily jog
- A reduction in elasticity of the vagina and thinning of surrounding tissue
- An increase in vaginal pH and decrease in healthy vaginal flora (aka: more infections, odors, and irritation)
- Increased skin disorders affecting the urogenital tract such as vulvodynia, vestibulitis, and dermatitis
- Pelvic prolapse symptoms (urinary leakage, pressure, and trouble eliminating)
And unlike hot flashes associated with menopause and aging, which eventually will end at some point even without treatment, vaginal dryness and these other symptoms usually increase in severity over time. (2)
What you may notice mentally:
- You may suffer from anxiety relating to worsening symptoms of dryness, discomfort or incontinence (Where is the closest bathroom? Will my panty-liner hold up? Why does it have to hurt so much?)
- You may be feeling older than your years
- Your self-esteem may be dwindling or literally in the toilet
- Your intimate relationship may be suffering due to either your physical discomforts during sex…or your fear of that discomfort
- You may suffer from decreased desire, arousal and orgasm – the decline in androgens are particularly associated with diminishing libido (3,4)
Dryness, discomfort and a little leakage…unfortunately…becomes the “accepted” norm! But does it really have to be that way?
I say “NO!”
And I’ll tell you why in a moment.
But first, let me address a question that I sometimes get from older women…and that relates to whether symptoms related to vaginal dryness are important for them to address…because, after all, they aren’t sexually active.
Let me just make sure everyone understands that even outside of sexual intercourse it is important to address vaginal discomfort. It is a quality of life issue but also has ramifications for your health as you age.
What negative impact can vaginal dryness have on your longer-term health?
- If you don’t address vaginal dryness you may see more urinary tract infections
- Vaginal and vulvar dryness can cause pain and discomfort outside of intercourse, while doing your favorite things (horseback riding, gardening, Zumba class, etc.) or even during your gynecological exam and/or Pap smear. Over the years when I had my practice I saw many patients who had tremendous discomfort even wiping due to the sensitivity of their vulva and surrounding tissue
- Vaginal dryness can be a warning sign of sorts relating to your declining hormone levels…your body is telling you that your “lady bits” need attention. These same declining hormones can cause urgency symptoms and even incontinence
- Lack of sex can actually create more dryness due to reduction in overall blood circulation in the vagina; healthy blood circulation can alternatively help counter dryness
Why most vaginal dryness treatment options are sub-optimal…
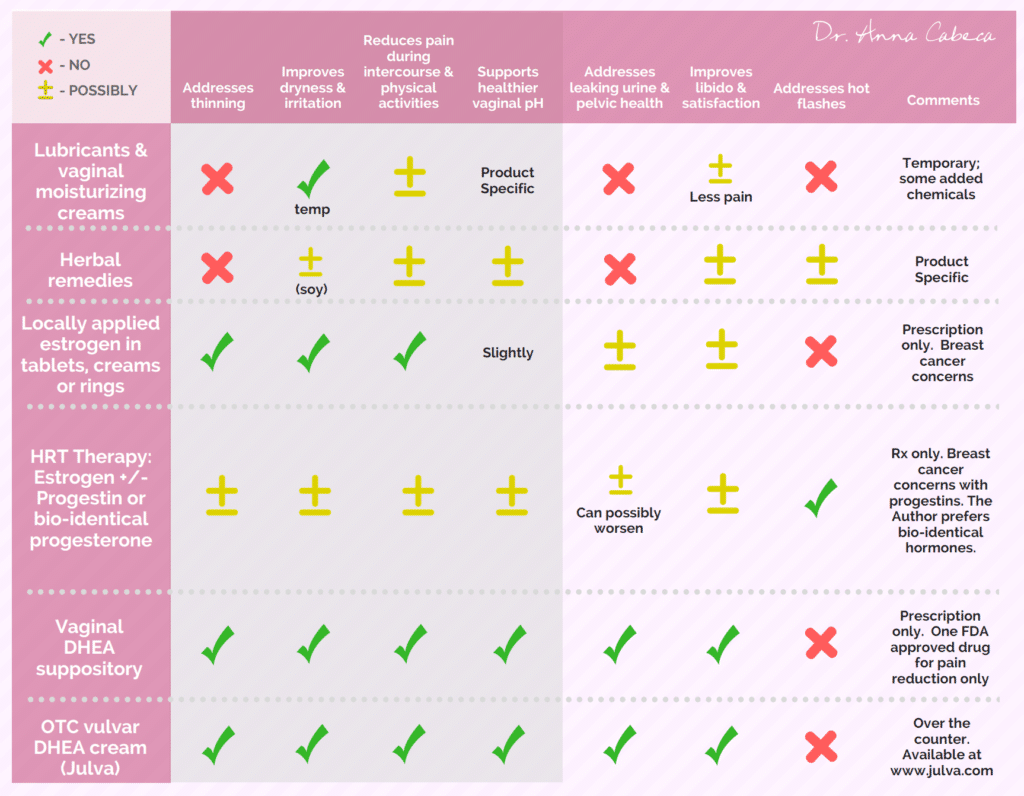
Current clinical treatment options for vulvar-vaginal dryness and atrophy are only partially effective in addressing the many symptoms that women suffer from! Treatment has been traditionally limited to over the counter (OTC) options, which may include lubricating creams and herbal therapies. Pelvic floor strengthening exercises are routinely recommended for vaginal atrophy but may not help significantly due to the degree of muscle loss. Medical prescriptions typically recommended are vaginal or topical estrogen and sometimes surgery as well.
Have a look – I created the diagram below to help you easily navigate the differing treatment options and better understand why some of the methods you may have tried in the past may have left you feeling frustrated or dissatisfied…
DHEA as a safe & effective vaginal dryness solution
While most medical research and available treatments have been focused on the effects of diminishing estrogen and testosterone, there is another key hormone that has been found to play an important role in addressing vaginal dryness and atrophy symptoms, and that is dehydroepiandrosterone (DHEA).
I want to share with you its use and in particular the scientific research and clinical findings that point to its effectiveness and safety and why it may very well be the solution you’ve been looking for.
But first, what is it and how is it produced?
DHEA is an androgen, similar to testosterone. Androgens improve many of the body’s functions. This includes the integrity and elasticity of skin, improvements in muscle growth and repair, and the health and strength of bone in both men and women.
DHEA also has a role in maintaining libido, sexual desire and sexual function. Androgens have also been shown to improve energy levels and mental alertness, provide cardiovascular protection by lowering cholesterol, and enhance bone building and repair by increasing calcium retention.
DHEA originates from the adrenal gland. It is an inactive precursor which leads to the production of active sex hormones like androgens or estrogens in specific cells and tissues. As estrogen levels naturally decrease it is DHEA that continues to be a remaining source of estrogens and androgens in a woman’s body.
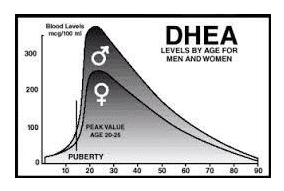
DHEA produced by the body naturally “extends” protective benefits to women as their estrogen levels decrease, but only for a time. There is a progressive decrease in serum DHEA which starts in the mid 20’s with an average 60% loss observed by menopause (5) as seen in the diagram below:
The great news for women is that while DHEA levels decline naturally over time, it can be introduced and utilized by the body after 30+ years of age to help slow our aging process and revitalize vaginal health.
Why topical DHEA is the answer…
While used for a variety of other health benefits, it’s important to know that oral DHEA has not been shown to address vaginal dryness and atrophy symptoms and has increased side effects. (6)
Research surrounding vaginally applied DHEA has shown that it can…
- Reduce vaginal dryness and irritation
- Have favorable effects on skin health and appearance (7) due to the production of collagen
- Strengthen vaginal musculature
- Increase bone mineral density
- Decrease pain during intercourse
- Increase arousal and libido, as well as sexual satisfaction (8)
- Transform DHEA to testosterone and the estrogen, estradiol (9) and this natural production of estradiol occurs without a significant release of estrogens systemically in the blood.
I along with other physicians have been able to write prescriptions for customized vaginal and topical DHEA and other hormones for decades with many positive results. Just this past November 2016 the FDA approved the first DHEA vaginal suppository to address pain during intercourse.
My own clinical experience using DHEA for vaginal dryness & atrophy
As an Emory-trained physician, I started using androgen therapy in my private practice in 1999. I used bioidentical DHEA and Testosterone vaginally or applied it topically to the vulvar area. Patients regularly came to me complaining of vaginal atrophy symptoms including vaginal dryness, irritation, pain during intercourse, and urinary leakage. Many suffered from libido issues.
I routinely achieved positive results with my patients for improvements to sexual health and vaginal dryness and a reduction in irritation and pain during intercourse. There were regular improvements in libido, arousal, and sexual satisfaction as well.
Some patients also reported decreased incontinence symptoms. Many patients seeing me for possible surgery due to pelvic prolapse and stress incontinence issues were able to avoid surgery altogether once I prescribed vaginal DHEA and testosterone to them!
For these patients, a physical examination confirmed their reported improvement – there were notable tissue improvements in the lining and within the vaginal ruggations (the normal folds and elasticity) as well as contractility (the ability to contract the muscles of the pelvic floor). This meant more strength, more support to the urethra and bladder too.
I wanted to be able to provide a non-prescription-based topical solution that provided anti-aging benefits. This would provide women all over the world with a less embarrassing option to address a significant quality of life and overall health issue associated with aging.
Three years of research along with my extensive clinical results led me to combine DHEA into a cream form with other quality natural ingredients having been shown to be beneficial to the skin and its underlying tissues. I called this feminine non-prescription anti-aging cream for the vulva, urethra, and vagina “Julva®”. 
New to the market, it already has hundreds of women providing heartfelt testimonials about how it has helped them physically and mentally…as well as sexually. Here are just a couple of stories of women having success with Julva…
In closing, what you need to know about DHEA & your “desert down under”…
So many women just deal with the symptoms of vaginal dryness by continuing to live with them, being unhappy, and in sexual distress. Even those who are not having sexual intercourse should know…there are treatments to help them live with less pain! I know many women who can’t even get a Pap Smear without great discomfort. And as women we all should know how to keep our pelvic floor healthy so as to not have to deal with prolapse issues and incontinence longer-term.
Let’s keep the conversation going about this life-affecting problem for women and the solutions that are now available. Vaginal dryness and atrophy due to natural hormone decline, aging, potential medication side-effects, childbirth, etc. do not have to be our new “normal” and it does not mean that we have to suffer in silence! Do your research. See if the use of topical DHEA is the right fit for you – try Julva!
And finally, ladies, please do not ignore or downplay the discomfort of vaginal dryness – it is a plea from your body signaling that it needs special care and attention! With time, your vaginal dryness issue can evolve into the quality of life challenges far more complex and painful than what you may currently be experiencing. Please take good care of your most sensitive feminine zone by paying attention to its signs and symptoms – it needs you!
Hormones Balance Women LOVE Julva!!
Please note that I am an affiliate for these products and do receive a small percentage of sales, but all opinions are my own.
References
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3845679/ and https://www.drugs.com/article/birthcontrolpill-risks-benefits.html
- J. Calleja-Agius, M.P. Brincat. Urogenital atrophy, Climacteric. 12 (4) (2009) 279–285.
- S. Leiblum, G. Bachmann, E. Kemmann, D. Colburn, L. Schwartzman. Vaginal atrophy in the postmenopausal woman. The importance of sexual activity and hormones. JAMA. 1983;249(16):2195-2198. Hormones.
- N.E. Avis, S. Brockwell, J.F. Randolph Jr, et al. Longitudinal changes in sexual functioning as women transition through menopause: results from the Study of Women’s Health Across the Nation. Menopause. 2009;16(3):442-452.
- Labrie F, Be´langer A, Cusan L, Gomez JL, Candas B. Marked decline in serum concentrations of adrenal C19 sex steroid precursors and conjugated androgen metabolites during aging. J Clin Endocrinol Metab 1997;82:2396-2402.
- R.M. Goel, A.R. Cappola. Dehydroepiandrosterone sulfate and postmenopausal women. Curr Opin Endocrinol Diabetes Obes. 2011 Jun;18(3):171-6.
- Available at: http://www.lifeextension.com/magazine/2010/12/new-research-substantiates-the-anti-aging-properties-of-dhea/page-02. Accessed January 2, 2017.
- F. Labrie, D.F. Archer, C. Bouchard, et al. Effect of intravaginal dehydroepiandrosterone (Prasterone) on libido and sexual dysfunction in postmenopausal women. Menopause: The Journal of the North American Menopause Society. 2009 Sept-Oct;16(5):923-31.
- Labrie F, Bélanger A, Bélanger P, et al. Androgen glucuronides, instead of testosterone, as the new markers of androgenic activity in women. J Steroid Biochem Mol Biol. 2006;99:182–8.
Dr. Anna Cabeca Bio:
Dr. Anna Cabeca is an Emory University trained gynecologist and obstetrician, a menopause and sexual health expert and international speaker and educator. She created the top-selling products Julva® – an anti-aging feminine cream for women, Mighty Maca™ Plus – a superfood hormone balancing health drink, and online programs: Magic Menopause, Women’s Restorative Health and SexualCPR. Read her blog at DrAnnaCabeca.com, and follow her on Facebook, Twitter and Instagram.
You can read about my own story and why that fed into my need to research and develop Julva®, or you can learn much more about Julva® here (along with more information as well as testimonials, you will find an extensive FAQ on the Julva® website).




How much is the Julva vaginal creme to purchase after trying the free sample size
HI Carole, here is a link to the full size bottle: https://order.julva.com/the-dream-cream
~ Jeanne HB Team
Need pricing
How do I purchase this
Hi Brenda, here is the link to the 7-day trial order page: https://order.julva.com/trial-pack?oprid=65383&ref=28126
~ Jeanne HB Team
Is this ok to use when you also suffer from melasma? I want cure to both, not one or the other.
Hi Jasmin,
It does not contain any endocrine disrupting chemicals. Julva® is an all-natural, anti-aging cosmetic cream for your delicate feminine parts. It’s been created by a Triple Board Certified OB/GYN — Dr. Anna Cabeca.
If you suffer with:
external vulvar thinning and irritation
dryness
burning and itching
painful intercourse due to vaginal dryness
vaginal and bladder infections
decreased desire, arousal and orgasm
embarrassing urine leaks
loss of elasticity/tightness/muscle strength within the vagina and urethra
lack of enjoyment of intimacy
lack of confidence and connectedness with our partner
It doesn’t have to be that way.
Have more questions? Check out the FAQ page with all the answers!
Julva FAQ: https://drannacabeca.clickfunnels.com/faq
~ Jeanne HB Team
I currently use Rx vaginal estrogen, would that be discontinued during use of Julia? I am interested in this product. How do I obtain it?
Hi Ann, here is the link to the 7-day trial order page: https://order.julva.com/trial-pack?oprid=65383&ref=28126
We do not recommend discontinuing any medication without your doctor’s guidance.
~ Jeanne HB Team
Hello. Can Julva be used if I am currently taking Bioidenticals Bi-est and Progesterone?
Hi Karen,
It may be best to discuss with your doctor, wether this product is a good fit for you. You. may also find the FAQ’s on this product and talk to Dr. Anna’s support team directly by clicking link above in article.
Healthy Regards,
HB Team
Is it safe for use for women who have had a form of uterine or endometrial cancer.
And also women on Tamoxifine for breast cancer?
Hi Terri,
Per Dr. Anna, if you are taking the prescription Tamoxifen, do not use this product. For more FAQ’s regarding this product, please click the link in the article above.
Healthy Regards,
HB Team
I am able to tell them I am aware of what they’re doing. I would absolutely suggest them on your next upkeep!
Hormonal suppositories? My friend had this issue and they were helpful.
Hi, I had a hysterectomy due to estrogen/progesterone+ ovarian cancer. Would it be okay to use Julva? I am not on any meds. Thank you
Hi CJ, we are not medical professionals, and so would recommend running it by your practitioner to see if it would be right for you. Take care! Jennifer
Hi from Spain, do you know any similar bran in Europe? I cannot find any, or at least vaginal DHEA? Thank you.