What You Will Learn in This Article
- What a thermogram IS and what it ISN’T
- The importance of – and the difference between – color and grayscale images
- Thermography and Estrogen Dominance
- The difference between thermography and mammograms
- What a thermogram can miss
- Which providers are good and what to ask before scheduling
- How to do a breast self-massage
- Benefits of working with a D.O.
- FAQs about thermography
- Where to start
In the last few decades, breast cancer has been a big concern for a lot of women. There’s a good reason for this, as breast cancer has been on the rise, along with other cancers.
But, is the mammogram really the best option for early detection?
Not necessarily—at least, not on its own. That’s why I want to introduce you to (or give you more information on) thermography.
Thermography is a safe, inexpensive, and non-invasive way to monitor breast health. I’ve known about thermography for a while, but to learn more, I interviewed an expert on thermography and breast health, Bruce Rind, M.D., D.O.. He gave me a great overview of what thermography is and how to make sure you get a good quality thermogram done by a qualified provider. This article is based on my conversation with Dr. Rind.
We’ll start out by covering what a thermogram is, and what it can be used for.
What a Thermogram IS and What it ISN’T
A thermogram is essentially a “picture of temperatures”. Picture your daily weather report on the evening news. The weather report shows northern states in blue because they are colder, and southern states in red, because they are much warmer. Now, there aren’t just two colors on the map. You’ll see oranges, yellows, and greens in between the hot and the cold.
Just as with the weather report, you’re looking at a map of the country, with a thermogram, you’re looking at a map of the person. The colors on a thermogram reflect the temperature of the breast tissue. Red, orange, yellow, green, and blue give you the temperature spectrum.
It’s important to note that a thermogram IS a Breast Thermal Findings Assessment. It is NOT a Breast Risk Thermal Assessment. The risk assessment comes from the doctor’s interpretation of the thermal findings, which may result in a diagnosis.
In other words, a thermogram is kind of like an x-ray. It’s nothing more than a radiological image of structures. It doesn’t diagnose. Just like when you get an x-ray, the black and white image itself doesn’t tell you whether there’s cancer there. It’s the interpretation that is the diagnosis.
The Importance of and Difference Between Color and Grayscale Images
While we might assume that having colors on a test would give us more information (especially when it comes to showing inflammation), there are some instances where using the gray scale is more appropriate.
Download the full Thermography Risk Scale PDF here.
Color is useful for seeing regional heat/temperature changes. The black and white scale, on the other hand, is much better if you want to see details that aren’t as visible on the color scale version. For example, while the black and white scale doesn’t show you actual blood vessels, it does give you a “thermo vascular pattern.” So, the darker lines that may look like blood vessels on the image are actually the heat given off by the blood vessels —just like on the color scale image, where the more intense color (red) indicates more heat.
A second thing is that the black-and-white image shows those leopard-looking spots better. Those spots are suggestive of Estrogen Dominance. You can’t see those on the color scale image because the colors are so intense. When you use both black-and-white and color scales, the thermogram gives you a good idea of what’s going on physiologically, rather than just anatomy-wise. It’s showing how the body is functioning.
That’s why it’s important to use both color and black-and-white scales for thermograms. In fact, when looking for a local thermography provider, I used this as one of the evaluation criteria.
Thermography And Estrogen Dominance
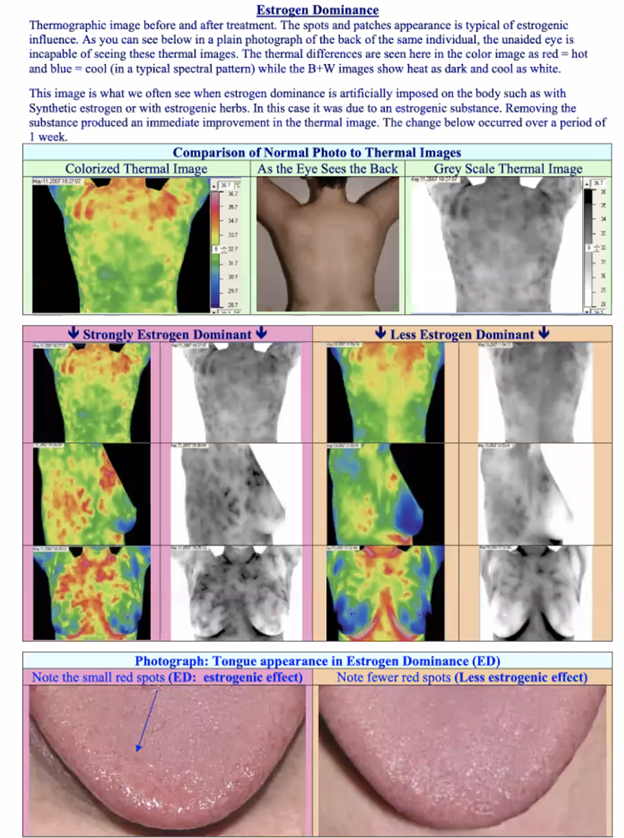
Thermography can be a great tool if you have Estrogen Dominance because there are noticeable differences in a thermogram when someone is strongly estrogen dominant. As mentioned above, the leopard spots that show up on the black-and-white version indicate higher estrogen levels in the tissues.
The tongue can also be a good indication of estrogen overproduction. In a situation of estrogen dominance, small red spots can be seen on the tongue, as seen in the photo on the left, above. With a normal estrogen level, you won’t see as many red spots, as seen in the photo on the right, above.
There’s a way to potentially find out which areas of the breast are estrogenic. It’s called the coffee challenge. Coffee makes the estrogenic areas of the breast stand out on the thermogram. It also warms up the breast in general, showing as red or orange.
Some women react strongly to coffee, to the point that their thermographic images become much more pronounced after simply drinking a cup of coffee. An “after coffee” image can look very similar to one that shows estrogen dominance with not enough progesterone to counterbalance it.
I have written about my reservations about women drinking coffee while trying to regain hormonal balance and how to recover from coffee addiction using alternative options (some include caffeine).
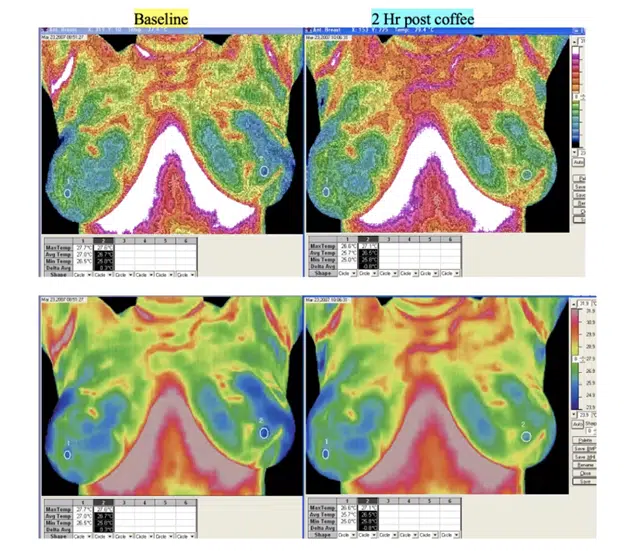
It doesn’t work that way for all women, but since it’s unpredictable, it’s better not to drink coffee before your thermography appointment. Of course, you could also do it purposely to find out which areas are estrogenic. To see the potential impact, check out the before and after coffee images below. (Look how much more red this woman has 2 hours after drinking coffee):
Source: Dr Rind’s medical practice.
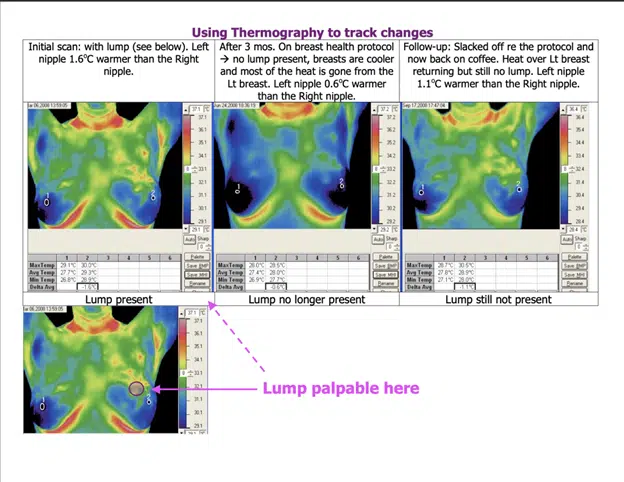
As you make dietary changes and supplement additions to address estrogen dominance, doing thermography along the way can help you to track changes in your breasts.
Difference Between Thermography And Mammograms
You might be wondering why you should do thermography when you can more readily get a mammogram. Here are some of the differences between mammograms and thermography:
The thermogram gives you a good idea of what’s going on physiologically in the body (way before cancer shows up), while the mammogram gives you an idea of structure, and what’s going on in the anatomy of the breast. A mammogram is like a chest x-ray, showing what’s there structurally, including a silhouette of the heart and ribs. You can see the structures, but you can’t tell from the x-ray whether the person is dead or alive. To know that, you’d need to perform an electrocardiogram (EKG). It may not look like the heart, but it tells you what the heart is doing. A thermogram is like an EKG for the heart, showing how the breast is doing.
While a thermogram may not show an actual tumor, it’s actually better as a detection method. Why? Because a thermogram can tell you if a tumor is on its way. So, it catches abnormalities a lot earlier than a mammogram.
What A Thermogram Can Miss
While thermography has many advantages over mammograms, there are a few conditions or issues a thermogram can possibly miss. It also doesn’t tell you whether or not you’re developing cancer. It just tells you how great the risks are.
Here are some of the things a thermogram can miss:
- Slow-growing cancers
- Calcification of the breast (associated with cancer)
- Inflammatory disease
- Cancers that are behind the breast but aren’t a part of the breast, like a tumor in the pectoral muscle (these are rare)
A thermogram simply gives you thermal images that a trained thermographer can look at and then tell you some of the associations and meanings of the temperature data. So again, it doesn’t diagnose anything or treat anything. It just gives you a picture of how the breast tissue is functioning.
How to Know Which Providers Are Good & What To Ask Before Scheduling
There are some things you should look for in a thermography provider, such as the following:
They Should Do the Cold Challenge
Dr. Rind recommends finding a thermography provider who does the “cold challenge” with each breast thermogram. To do a cold challenge, a practitioner places gloved hands in cold water and then places them on the breast to trigger a “chill response” from the breast tissue.
This helps the thermographer to better distinguish healthy tissue from unhealthy tissue. Healthy areas tend to have a uniform cooling response, whereas cancer and inflamed areas either don’t cool or may become warmer instead. So, the chill response of healthy vs. unhealthy breast tissues is clearly different.
However, if the breast tissue fails the cold challenge, it doesn’t necessarily mean cancer is present, it just makes that area a bit more suspicious.
Room Temp at 68 to 72 Degrees
The room temperature for the thermography scan should be within the range of 68 to 72 degrees Fahrenheit. If it isn’t, it could cause the patient to either shiver or sweat, which can change the results. The relative humidity should also be under 70% so that there is no moisture build-up or sweating on the skin.
Resolution Should be As Per These Guidelines
It’s also important to have the correct resolution when getting your thermogram done. According to their listed guidelines, the AAT recommends a detector resolution of greater than 640 X 480 pixels with an appropriate microbolometer and lens.
However, if the imaging system has a detector in the 320 X 240 pixel range, it may still give you a good image, resolution, and spot measurement, as long as it has a high-quality microbolometer, lens, and software or technology that is designed to compensate. The smallest spot you should be able to see with this resolution is about 2X2 millimeters.
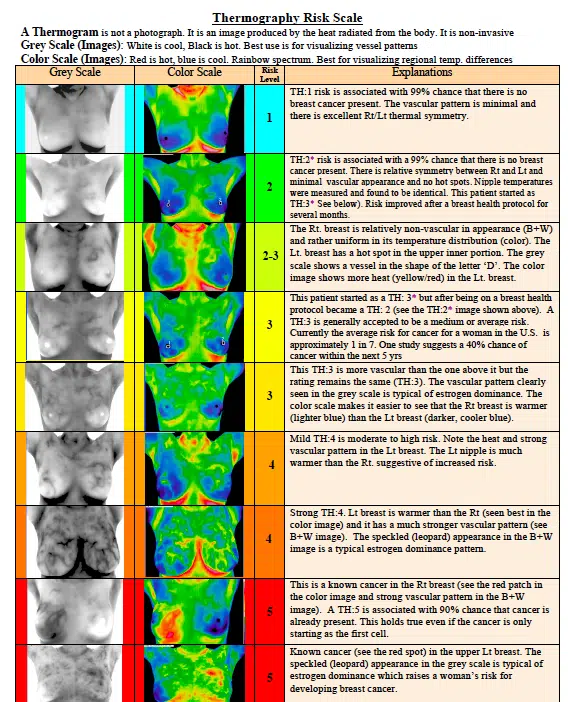
TH Scale Should Be Used
The TH scale is an established classification system used in reporting findings. The “TH” refers to the Thermographic risk level. Thermo Biological classification is a grading system, and these are the “grades” you can get, starting with TH-1 as an “A” for healthy breasts.
- TH-1 — Lowest risk with 99% certainty that no cancer is present
- TH-2 — 99% probability that no cancer is present
- TH-3 — Up to 40% chance of developing cancer within 5 years
- TH-4 — Moderate to high risk of developing cancer
- TH-5 — 90% probability of cancer already present
The results of the thermogram are just findings. Any abnormal results mean you should make an appointment with your doctor or breast health practitioner for a diagnosis.
Thermal Resolution
During the thermography exam, the practitioner will look for symmetry between the left and right breasts. That’s a really important criterion for evaluating breast health. Any suspect areas should be measured at a thermal resolution of at least 0.1 degrees Celsius to measure the risk level.
Color Scale and Grey Scale
The provider should include both color scale and grey scale for the reasons mentioned earlier. If both images aren’t included, you’re only going to get a partial picture of what’s going on. The eyes pick up on some things better in color and other details better in black and white. So, getting a thermogram with both color scale and grey scale gives you a thorough report of findings.
Temperature – Record It and Assess
The specific temperature of the breast tissue should be recorded on the images, especially on suspicious sites. This is supposed to be a measurement, so just “eyeballing it” isn’t good enough. The practitioner should include the temperature readings with your image results.
Member of AAT or Trained By Them
Ideally, your thermography provider should be a member of an organization called the American Academy of Thermology (AAT) or should have been trained by the AAT. This is the premier organization for thermography training. They adhere to the highest standards internationally, under the excellent leadership of their director, Robert G. Schwartz, MD.
You can find a member provider near you by going to this link.
How To Do A Breast Self-Massage
One of the best things you can do for your breast health is a regular breast self-massage. This can help move lymphatic stagnation and can be used as early detection. I first learned about this technique from holistic breast health practitioner, Gaye Walden of Holistic Breast Health. She is the one who introduced me to Dr. Rind.
While massage, in general, is helpful for activating blood flow and the lymphatic system, there’s a type of massage that is designed to target the lymphatic system of the breast. It’s easy to do yourself, and you can do it while taking a shower, or by incorporating our Happy Sisters topical breast cream in your lymphatic massage.
Here are my breast massage tips:
See image below
- Massage in the shower when wet, soapy, and slippery.
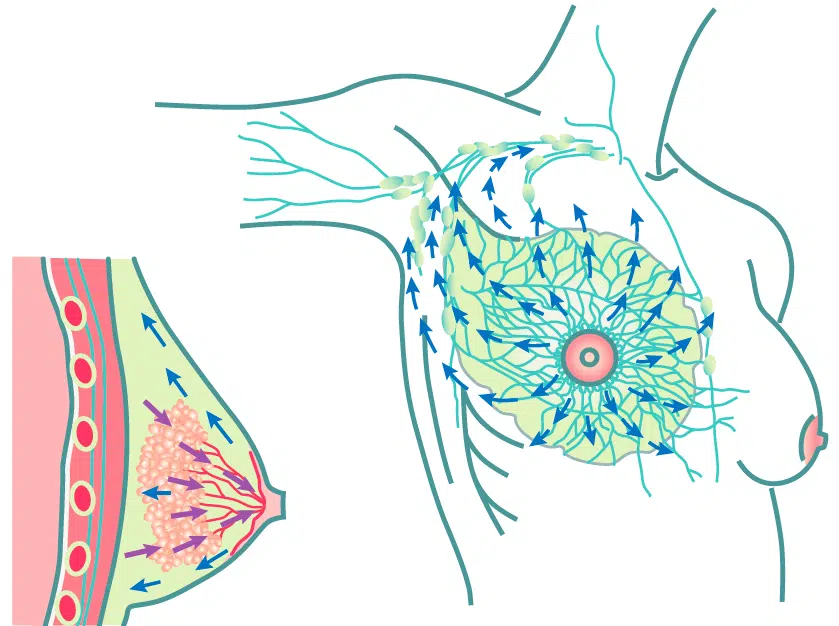
- Use your open hand to sweep in the direction of the lymphatic flow (see arrow directions in the picture below).
- Sweep from nipple toward 12:00, 2:00, 4:00, 6:00, 8:00, and 10:00, two times per breast.
- Go slow, about three to five seconds per sweep, and go gently deep.
- Massage with your opposite side hand.
- Visualize the breast as being made of a sponge containing thick honey. Slow, deep sweeps make the honey flow out.
- Visualize your breast being nourished, cleansed, and healed.
I’ve recorded a video with a breast specialist that shows you exactly what to do. You can access the video at this link. However, you may prefer to work with a manual lymphatic drainage (MLD) specialist or an osteopath.
Benefits Of Working With a D.O. (Osteopath)
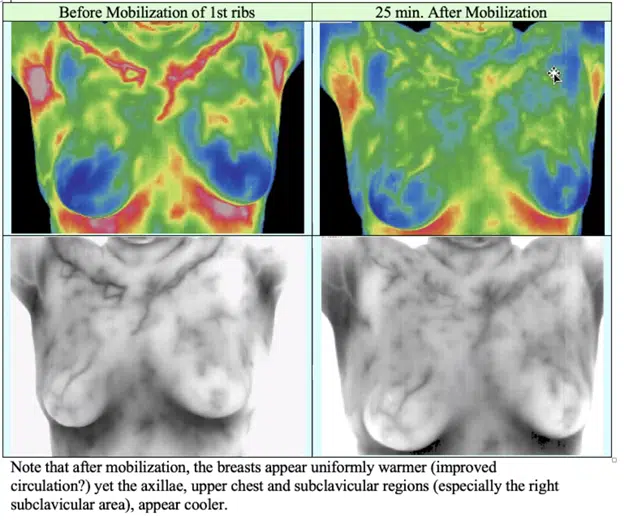
While breast self-massages are really helpful, there are advantages to working with a medical doctor who is an Osteopath. Osteopaths can help with gentle body part manipulation, which can help improve the lymphatic movement in the breast. Rib mobilization can be especially helpful. You can see the before and after of rib mobilization in the images below:
However, it’s important to find an osteopath who specializes in working with their hands and is comfortable doing musculoskeletal work. Such a provider can work with subtle changes in the body like rib mobilization.
FAQs About Thermography
Q: Does a “hot spot” always mean there’s cancer there?
A: No. Sometimes a “hot spot” is a dimple that’s capturing heat because of previous surgery or some other cause, like inflammation, an infection, healing scars, or a benign tumor. That’s why it’s important for a practitioner to get a good history and do a thorough exam.
Q: Who can benefit from thermography?
A: Whereas mammograms are generally recommended for women over 50, thermography can be used by women of all ages. I’m personally committed now to getting a thermogram yearly.
Q: Do men have breast issues as well, that could use thermography, or is this just a women’s thing?
A: 99.9% of thermograms Dr. Rind has done are on women, but it’s rare for him to do men.
Q: Is it possible to work with Dr. Rind?
A: Yes, Dr. Rind works one-on-one with patients at his office in Gaithersburg, Maryland, which is just outside Washington D.C.. You can read more about him by going to his website, www.drrind.com.
Q: Is thermography a standalone assessment if you want to keep tabs on breast health?
A: Not necessarily. If your thermography indicates high risk, you may also need to pursue mammography, an ultrasound, an MRI, or even a PET scan.
Where to Start
If you’re interested in improving and tracking your breast health naturally, here’s where to start:
- Schedule your first thermogram as an early detection method, following the guidelines for finding a provider above. You’re looking for:
- Provider who does the “cold challenge”
- Room temperature range of 68 to 72 degrees Fahrenheit.
- Resolution of greater than 640 X 480 pixels
- Use of the TH (Thermo Biological) classification system for results
- Thermal resolution of the thermogram should be____
- Use of both color scale and greyscale
- Temperature should be recorded on the images
- Member of the American Academy of Thermology (AAT) or at least trained by them
- Make sure you’re eating an anti-inflammatory diet, as outlined in my book, Overcoming Estrogen Dominance. It’s also a good idea to limit or avoid coffee and alcohol.
- Learn to give yourself a breast massage. This video will guide you through the process. You can also purchase a kit, called My Breast Friend™ which gives your fingers training on what to feel for. The kit includes a silicone breast model, an instruction booklet, and an instructional video. It can help you find abnormalities as small as a pea. The Wellena Happy Sisters Kit also includes a topical breast cream to support lymphatic breast massage; the cream includes medicinal herbs and oils known for their ability to support the lymphatic system and reduce the pain associated with fibrocystic breasts.
Learn more with Overcoming Estrogen Dominance
“The body has an amazing ability to heal. We just need to give it the right resources.”
In Overcoming Estrogen Dominance, my goal is to empower and give you the tools to take control of your hormones and health.
More than 70% of women experience estrogen dominance. The symptoms range from lumpy and fibrocystic breasts to thyroid nodules, hot flashes, fibroids, uterine polyps, painful, heavy or irregular periods to infertility and miscarriages, from mood swings to insomnia, weight gain to fatigue.
So many women have experienced the pain and frustration that comes when they feel their symptoms and complaints are dismissed or minimized. This is particularly true for women who are experiencing the symptoms of hormone imbalance. Even when doctors do offer treatment, it’s typically in the form of prescription medication or invasive surgical procedures.
In Overcoming Estrogen Dominance, I hope to show that those extreme interventions are often unnecessary and to give women a roadmap to reverse estrogen dominance using food, herbs, supplements, and natural protocols to rebalance hormones.
To get your copy of Overcoming Estrogen Dominance, go here.
Disclaimer
These statements have not been evaluated by the Food and Drug Administration. This product is not intended to diagnose, treat, cure or prevent any disease.
Resources
- Rind, B. (June 2021). Thermography Interview. Via Zoom.
- American Academy of Thermology. (2019). Guidelines. AAT website.






Hi Rosemary-Thank you for sharing your story. Please email [email protected] to get some resources and help with finding a practitioner in your area! We’d be happy to help. ~HB Team
Rosemary, please look up MELT method for your joint stiffness. meltmethod.com. It’s a technique that you can do at home to increase mobility and fascial hydration.
Thank you for such a wonderful explanation of Thermpgraphy. It was so informative.
Looking for thermography internationally?
https://thermologyonline.org/find-a-clinic/
Just pop the country name in to search
You should see Dr. Veronique DeSaulniers! She is a breast cancer conqueror! She helps you w/treatment plans, She also has a great book called “Heal Breast Cancer Naturally”
https://www.breastcancerconqueror.com
She’s excellent!
how can I learn the breast health protocol?
I’ve done yearly full-body thermograms since 2016. In spite of a strong history of cancer in my family – especially breast cancer – my thermograms show that my breasts appear to be the healthiest part of my body and that very little has changed since starting these annual images. I’m always relieved to get the results.
Hi Kd, this is great to hear! Thank you for sharing. ~HB Support
I’ve been doing breast thermography for about 15 years and I just found a breast lump, not due to thermography detection, and after a mammogram and ultrasound, it was determined that biopsies were necessary… I guess I’m surprised that thermography wouldn’t have caught it at my last exam eight months prior.
Hi Nance, that is interesting, thank you for sharing with us. It’s great that you sought out different modes of testing, this can be important. HB Support
Hello! We’re proud to have thermography in our office! Come see us soon!
Therapeutics & Thermography Inc
6633 N. Mesa Suite 513
El Paso, TX 79912
(915) 401-4053
I’ve been using thermography to monitor breast health for about 10 years, never had a mammogram. I’ve been trying to determine if or where mammography fits into the picture. Definitely it should be used if any questionable results show up on the thermogram, but as an adjunct routine screening tool, does it need to be used and how often?